By Claudio Lehmann, MD
This piece was originally published in the March/April issue of the Tarrant County Physician. You can read find the full magazine here.

We can all learn in many ways from the intellect of Greece and Rome. This principle applies to infectious events which took place in those societies in the long distant past and were well documented by ancient writers in their descriptions of early epidemics.
In these difficult COVID-19 times we still rely on these empiric approaches obtained from past management of epidemics in times of war and peace. We have also learned how to complement this management with careful scientific research and study to develop more specific treatments and successful vaccination programs. Additionally, we have learned that it is important to have consistent, well-coordinated public education.
The Athenian Plague
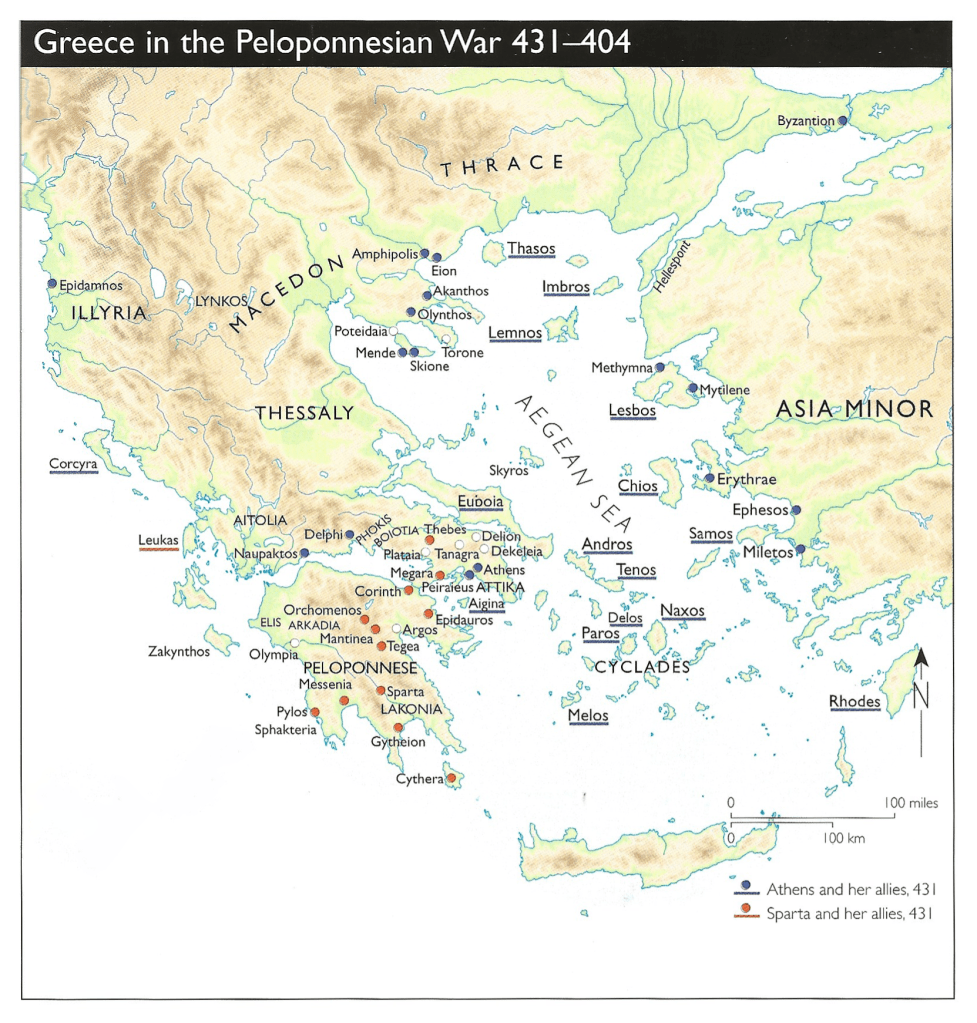
This plague occurred in the setting of the Peloponnesian War, a long war caused by conflicts between the states of Athens and Sparta and their allies.1,2,3 Democracy originated in Athens in 500 B.C. It was brought about through the assembly of the 500, a group chosen to make important decisions regarding essential affairs of the city.
Athens, expanding into Attica and controlling the surrounding Ionian Islands, established the Athenian (also called Delian) League and built a naval empire. It became wealthy by exporting olive oil and wine and trading silver from nearby mines. It thrived under Pericles, a leader who built the Parthenon and encouraged culture and creativity in the city.
Sparta, by contrast, was a land-locked military state comprised of rigorously trained soldiers. It was ruled by kings that controlled underclass servants. They also expanded into neighboring city-states. Athens and Sparta became rivals that clashed due to their different styles of government and policy.1,2,3
The Spartans also built their own defensive alliance, the Peloponnesian League, which antagonized the Athenian League.
Athens protected its neighboring states from Spartan attacks and built walls between Athens and Piraeus (also spelled Peiraieus). To prevent further clashes Athens and Sparta signed a peace agreement, but the Spartans and their allies disliked the democratic and expansive Athenian approach and felt it needed to exercise greater restraint. Therefore, in 431 B.C., Spartan troops and allies made several incursions through Attica into Athens. This started a long series of battles with inconclusive results that were fought for 26 years in different sites either by land or sea. This ruined the Greek economy, adversely affected the lives of many families, and changed the course of Greek history.
This so-called Peloponnesian War has been described at length by the brilliant general and historian Thucydides and is still studied by contemporary researchers.1,2,3 The final downfall and cultural deterioration of Athens was caused by the combination of damage to its fleet after a failed invasion of Sicily and by the enormous loss of life caused by the Athenian plague.
This epidemic started in the second year of the Peloponnesian War, after the Spartan invasion and siege of Athens in 430 B.C. As reported by Thucydides, this disease appeared suddenly, with high fever, red eyes, sore throat and tongue, hoarseness and cough, vomiting bile, severe diarrhea, restlessness, purplish cutaneous pustules and ulcers, and also lesions over fingers and toes, sometimes with gangrene. Recent review articles suggest that the most likely epidemiological diagnosis was smallpox, with typhus being less probable.5 It did not appear to be bubonic plague.
Thucydides described the overcrowding in the walled city of Athens where he proposed the important concept of contagion of disease. He defined it as the transmission of illness from a sick person to a healthy individual. He was then influenced by the ideas of Hippocrates, who claimed that the secretions of a sick individual would contaminate the air during an epidemic.6
This proposal anteceded by thousands of years Pasteur’s and Koch’s observations on germ transmission. Thucydides also noted that death could occur on the seventh or eighth day of disease but observed that those who recovered might acquire partial immunity and did not die from a second round of disease.
Waves of infection affecting the local population led to the death of one-third of Athens’ inhabitants. So many of the dead remained unburied that at times the corpses piled up on the street. Thucydides blamed this on lack of humanitarian response of the survivors. He himself, who got the disease and recovered, suggested avoiding overcrowding and exposure to the sick; however, Pericles, who was leading Athens at the time of the infection, suggested the transfer of rural refugees to the walled city. This increased the risk of their contagion. He also became a victim of the illness, from which he did not survive.
Euripides, who also lived at the time of the war in 415 B.C., described in an allegorical drama, “The Trojan Women,” a prophecy for a tragedy that predicted the disaster that would befall Athens after the failed Sicilian campaign when Athens lost her entire fleet, and a large number of young sailors became enslaved. This was a message on bad war planning in a Greek drama written in the fifth century B.C.7
As Rome conquered Greek territories, the Roman Empire in turn was deeply influenced by Greek culture, which became integrated into buildings and sculptures. The Roman Empire was also influenced by their religious beliefs and images. Hellenistic centers created in Alexandria and in cities of Asia Minor were later absorbed and integrated into Rome.
Antonine Plague
The first recorded epidemic in Roman times was called the “Antonine plague.” It appeared in A.D. 165 to 180, and waves of disease followed between 211 and 266. To Galen, the observant Greek physician, the victims presented with fever, chills, sore throat, bloody diarrhea turning black, and a pustular rash on the ninth day consistent with smallpox. The acute phase of the disease lasted two weeks. It affected large numbers of Roman residents, with high mortality due to the density of population and excess of waste and sewage.4 It killed Marcus Aurelius Antoninus and Lucius Verus, the two reigning emperors.8 It is believed that the Roman soldiers brought the organism from Egypt and the Middle East into Rome.
In those times, early Christians were persecuted for refusing to honor the Roman gods. However, they endeared themselves to the sick for providing them with some form of care.
The Roman Empire later became stretched financially by excessive warfare, rapid emperor turnover, and increased civil wars. Rome was eventually sacked by invading Visigoths in 410, and the last western emperor was deposed in 476 A.D.
Justinian Plague
The Eastern branch of the Roman Empire was then established with Constantinople as the capital of what was to become the Byzantine Empire. A different type of plague appeared in 541 A.D. during the Emperor Justinian’s rule in Constantinople. Justinian (527- 565 A.D.) is known for military campaigns, civil law reforms (he wrote Codex Justinianeus), and for creating important buildings (Hagia Sophia in 562 A.D.).
It has been claimed that this plague caused the loss of up to one-third of the total Mediterranean population. It may have presented in recurrent intermittent waves that, lasted up to 200 years. It has also been suggested that it led to the waning of the Roman Empire and the advent of the Middle Ages.11
The historian Procopius (500 – 565 A.D.) described the appearance of this plague in Pelusium, Egypt, on the Eastern Nile, and its spread to Alexandria and later to Constantinople, Asia Minor, and the Middle East.
Procopius observed subjects with fever. They had “large painful swellings” in groins, armpits, and neck followed by delirium, black blisters, and vomiting, which frequently led to death. Occasionally, he noted, “The lumps start draining pus, the fever subsides, and the person sometimes may even recover.” There were similar reports from other observers at that time, like John of Ephesus.8
We know now that rats carrying fleas were brought in by ships supplying grain from Africa to Constantinople. Bubonic plague’s causative organism, Yersinia pestis, has been isolated and its DNA sequenced.10 This was obtained from tombs in sixth century Bavaria. It was found to represent a distinct genetic lineage originating from a different rodent reservoir for this pandemic than the one occurring in medieval Europe.
A recent detailed research paper by a multidisciplinary group questions the Justinian plague as being such a watershed event in history.9 After examining a series of independent fields of study such as papyri, inscriptions, and coins as well as pollen and burial sites, the authors conclude there is little evidence that the Justinian plague was a major driver of demographic change in the sixth century Mediterranean area. These findings indicate this plague was therefore very different from the devastating second pandemic that presented later in the Middle Ages.
We have learned that two ancient pandemics, the Athenian plague in early Greece and the Antonine plague in early Rome, appeared in cities with overcrowded populations. Their disease presentation at the time indicated exposure to a highly infectious, rapidly spreading agent that caused an acute, devastating disease of high mortality. Both epidemics had similar clinical presentation, in which fever and mucosal and pustular skin lesions predominated. We know now that they most likely represented smallpox, and this disease became airborne from mucosal lesions but could also spread by contact of skin ulcerations. It affected people of all social classes, including leaders and emperors. Such a contagious disease would have made patient care very risky and difficult. No wonder the corpses piled up on the streets of Athens!
Smallpox ravaged the entire world. It reached the Americas, including the U.S. and Mexico during colonial times. It decimated the Aztecs when the Spanish conquistadors arrived in Tenochtitlan, as the Aztecs had no previous exposure to this virus.
After Jenner published his spectacular results with vaccination in 1798, smallpox immunization was eventually adopted all over the world and the disease was completely eradicated by 1980.
Prevention of social gatherings was applied during the severe 1918 flu pandemic with measures such as closures of schools, shops, and restaurants, mandated social distancing, and home quarantining when needed. In cities in which these multiple recommendations were implemented earlier and kept in place, transmission of disease and mortality were reduced. This beneficial result demonstrates that avoidance of contact between individuals can be helpful in controlling transmission of highly contagious disease, which is why this approach is being used for the management of the COVID-19 virus.
References
1RMorkot-HistAtlas Ancient Greece-
Penguin 1stEd 1996
2D Kagan – The Peloponnesian War –
Viking 2003
3VHanson-A War Like No Other-
RandomHouse2006
4ErinyHanna-Cities,Disease,Trade,
Epidemics in Roman Empire
Vanderbilt-Uni 2015
5RLittman-The plague of Athens.
Epidemiol and Paleopathology.
Mt.SinaiJMed 76:456
6HippocraticWritings:The natureof man
Penguinclassic1983
7Euripides TheTrojan women Signet classic 1998
8GKohn; Encyclopedia of Plague and
PestilenceWordsworth1995
9LMordechai-The Justinian Plague An Inconsequential Pandemic? PNAS 116-5125546
10D Wagner – Yersinia Pestis and the Plague – Genomic Analysis Lancet 14 April 2014
11Bassareo – Learning from the past in Covid-19 Era – Post Grad Med J 114:633
Images
1Souza, Philip De, The Peloponnesian War, 431-404 BC., (Oxford: Osprey, 2002).